Recent suicide bombings and other attacks within Israel are turning that country into a world leader in disaster management.
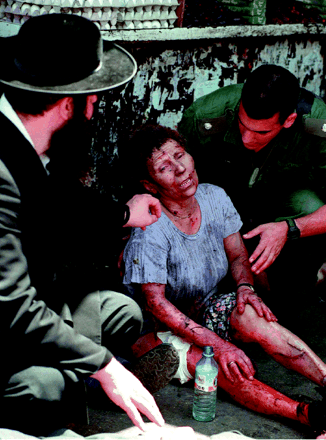
Figure. Woman receives aid after an attack by a suicide bomber in Israel Photo by: Canapress
The latest refinement involves an increasingly common problem. In a country with over 6 million residents, how can seriously injured people with no identification be identified if they cannot communicate with rescue personnel?
Israeli emergency officials have responded with an electronic network linking hospitals throughout the country. A few months ago, they began taking pictures of unidentified victims and/or belongings immediately after an incident. These are then transmitted across the country.
Shmuel Reznikovich, a representative of the Israeli Ministry of Health, told the Second International Conference on Urban Health in New York in October that the process allows anxious relatives to visit local hospitals, where social workers show them the pictures.
During a panel presentation on urban disasters, Reznikovich and some colleagues described the ways Israel has attempted to deal efficiently with its recent spate of multicasualty disasters. Gili Shenhar, a retired colonel and senior adviser in emergency and disaster management, explained that the media now plays a key, if unofficial, role at every disaster scene because their reports are “the only way to get to every family in real time, and to give guidelines.”
Not only do the reports “make the public feel more secure because the situation is under control,” added Doron Kotler of Magen David Adom, the country's emergency services organization, but they also mean that fewer people flock to the scene and hamper emergency personnel. When there are bystanders, “we often navigate them to our benefit” by putting them to work as stretcher bearers.
Although the response to disasters is coordinated by the police or, for larger incidents, by the Home Front Command responsible for civil defence, the Ministry of Health has overall responsibility for medical readiness.
At the hospital level, specific staff are available to handle major disasters, while all staff will be aware of guidelines, said Reznikovich.
“We have learned that effective primary evacuation is crucial in light of the complexity of relocation,” he said. Emergency personnel attempt to send critically injured patients directly to the hospital best suited to their care, since having to transfer them later will waste resources.
But the danger doesn't subside even after the bombs have gone off. Ambulances and police officers are blocked from coming directly into hospitals — all must be checked first because of the risk of hijackings and disguises.
At the site of an emergency, said Kotler, rescue work begins immediately, despite personal risk. He cited a building collapse in 2001 in which 339 of 650 guests attending a wedding were injured and 23 killed, and 75% of the casualties were evacuated in less than an hour.
The final step is identification of the dead. Today, all unidentified bodies are sent to the National Forensic Medical Institute for identification by DNA testing or other methods. This routine was established because of some incidents in which several families attempted to claim the same body. — Ann Silversides, Toronto











