Surgical “damage control” techniques developed at US urban trauma centres to keep victims of multiple gunshot wounds alive are now being used to save the lives of soldiers injured in Iraq and Afghanistan.
The military use of techniques pioneered in American inner cities is a reversal of the usual historical pattern, in which war has stimulated medical advances that subsequently found application in the civilian world.
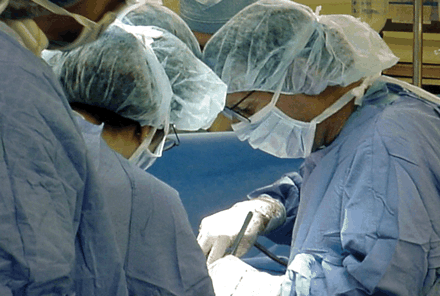
Figure. Dr. Schwab (right) recently used his “damage control” technique on Canadian soldiers. Photo by: Hospital of the University of Pennsylvania
“It's a real paradigm shift,” said Dr. C. William Schwab, chief of traumatology and surgical critical care at the Hospital of the University of Pennsylvania and professor of surgery at the University of Pennsylvania School of Medicine. “The history of trauma surgery has been a history of war. [Now] so much of what is going on in Iraq is being modelled after American urban trauma centers.”
Schwab recently completed a stint as a senior visiting-surgeon at the US Regional Medical Center in Landstuhl, Germany, where he operated on wounded US and Canadian soldiers. He is the first to serve in the volunteer program developed by the American Association for the Surgery of Trauma and the American College of Surgeons' committee on trauma.
Many of the techniques of damage control surgery were developed in the late 1980s and early 1990s at urban trauma centres after the introduction of 9-mm semi-automatic pistols in the US led to an increase in the number of young men with multiple penetrating wounds.
Taking the time to perform definitive surgery immediately often resulted in “a fully repaired but dead patient.” Schwab and his colleagues instead began to use abbreviated resuscitative surgery to halt the downward spiral associated with the lethal triad of acidosis, hypothermia and coagulopathy, which often develops in the catastrophically injured.
To control bleeding from damaged vessels or restore flow where needed, they inserted plastic tubes or vascular shunts, “like a quick fix in a broken plumbing system,” said Schwab. They clamped, stapled or sutured bowel ends to control intestinal spillage and contamination. After packing all raw or dissected surfaces, they then temporarily closed the abdominal or chest wall.
Patients were then moved to intensive care. After restoration of normal physiology and re-examination of all injuries, the surgeons then did definitive repair surgery a day or so later.
In a retrospective review of medical records of 22 patients with penetrating abdominal wounds with combined major vascular injury and 2 or more visceral injuries (J Trauma 1993;35:375–83), the damage control techniques could have resulted in a survival rate of 77% compared with 11% using the usual (definitive laparotomy) techniques. A 2000 review article (J Trauma 2000;49:969–78) found a survival rate of up to 60% across several studies.
During his Navy days, Schwab had observed a “damage control” call on an aircraft carrier, and watched the ship's crew rush into a flooding compartment to seal the damage.
The steps that surgeons take to save life while restoring physiology were also best described as “damage control,” Schwab decided. The strategy, which defied the traditional approach, has been hailed as a major advance in surgical practice, and its use has spread beyond abdominal injuries to cross all surgical disciplines.
Most recently, wounded soldiers in Iraq or Afghanistan have undergone damage control in-country by forward surgical teams. The wounded are then quickly transferred to a US military hospital in Balad, north of Baghdad, usually just for a day. They are then airlifted to Landstuhl — some arrive within 24 hours of being wounded — for stabilization and to begin definitive care.
Schwab wonders if, in another 20 years, damage control will pass into surgical history like ultra-radical mastectomy or truncal vagotomy, as physicians learn how to prevent the downward physiological spiral that makes it necessary. “One can only hope,” Schwab concluded.