A 25-year-old woman was admitted for weakness of two month’s duration. She had been diagnosed with anorexia nervosa (binge-eating/purging subtype) at the age of 21 years. She had a history of repeated admissions for hypokalemia caused by self-induced vomiting and abuse of laxatives. On examination, her body mass index was 14.3 kg/m2. Laboratory values showed a serum creatinine level of 51.3 (normal 18–106) μmol/L, a serum potassium level of 1.6 (normal 3.5–4.9) mmol/L, a high urine chloride level of 101.4 mmol/L and a very low urine calcium level of less then 0.5 mmol/L. After discussion about the laboratory results, the patient admitted to using thiazide before this admission. Renal ultrasonography (Figure 1) showed marked medullary hypertrophy in both kidneys, the hallmark of chronic tubulointerstitial nephritis.1
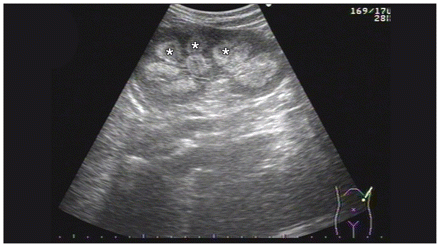
Renal ultrasonography image of a 25-year-old woman with anorexia nervosa, showing markedly hyperechoic rims along the outer medulla without accompanying shadowing or papillary necrosis (asterisks).
Chronic hypokalemia is commonly caused by purging behaviours or abuse of laxatives or diuretics. It can cause hyperplasia of the renal tubular cells and eventually tubulointerstitial fibrosis and progressive loss of renal function — namely, hypokalemic nephropathy.2 Although eating disorders are present in around 30%–40% of patients with hypokalemic nephropathy, the prevalence of hypokalemic nephropathy in people with eating disorders is unknown.2
The level and duration of hypokalemia necessary to develop hypokalemic nephropathy is unclear. Of note, use of diuretics is not a risk factor for hypokalemic nephropathy as long as chronic hypokalemia does not occur. The early stage of hypokalemic nephropathy is usually reversible with potassium replacement, but persistent hypokalemia leading to tubulointerstitial nephritis and associated renal failure may be irreversible.3 Mortality in severe instances of eating disorders is more commonly a result of arrhythmia or suicide, rather than a consequence of hypokalemic nephropathy.3
Footnotes
-
Competing interests: None declared.
-
This article has been peer reviewed.