A majority of Canada’s family doctors are worried about their inability to access publicly funded physiotherapists and occupational therapists, hospital beds, magnetic resonance imaging (MRI) machines and positron emission tomography (PET) scanners for their patients, according to the 2013 National Physician Survey.
“The message we want to convey is our concern for patients having timely access to therapy, and the role that family physicians play in helping them access that care,” says Dr. Francine Lemire, executive director and CEO of the College of Family Physicians of Canada.
Access to publicly funded physiotherapists was a major concern for 79% of family doctors, and 71% were unhappy about the difficulty of securing appointments for patients with publicly funded occupational therapists. More than half of all family doctors reported unsatisfactory access to hospital beds and MRI scans (57% and 53%, respectively), and 60% were unhappy about the difficulty of securing PET scans.
Difficulty accessing publicly funded rehabilitation therapists could reflect growing demand by aging Canadians, as people recover from strokes and joint replacements, Lemire suggested, in addition to the regular demands on the system to address work-related injuries and other illnesses.
The College of Family Physicians, the Royal College of Physicians and Surgeons of Canada and the Canadian Medical Association surveyed 60 021 practising physicians, with 10 487 responding to questions on topics ranging from workplace to patient care issues. The survey is considered accurate within plus or minus 1%, 19 times out of 20.
“Canada’s doctors know that we need to make changes now to respond to the evolving health care needs of our aging society,” Dr. Louis Hugo Francescutti, president of the Canadian Medical Association, said in a statement. “As a first step that means we need our federal government to lead the development of a national strategy for seniors’ care in collaboration with the provinces and territories.”
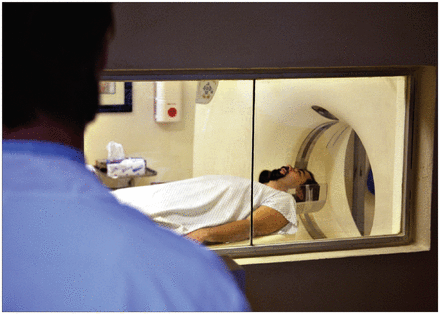
Timely access to MRI machines and PET scanners are among Canadian physicians’ concerns.
Image courtesy of © 2013 Thinkstock
In addition to concerns about lack of access to treatment for patients, some specialists — including neurosurgeons, dermatologists and pathologists — indicated a major increase in requests for their services. Not surprisingly, given Canada’s aging population, 59% of geriatric medicine specialists reported an increased demand for their services over the past two years.
On the work front, doctors spend an average of 54 hours a week caring for patients, conducting research, teaching or performing administrative tasks. Most clinicians provide an average of 110 hours a month of on-call services, as well as regular practice hours, the survey indicates. Doctors working in Saskatchewan and Manitoba worked the highest number of hours each week, at 61 and 58 respectively, with doctors in Quebec and British Columbia reporting they worked 53 hours a week, slightly less than the national average.
The survey also indicates the gender gap is closing in terms of male and female physician workload, with female doctors working five hours fewer a week than male doctors, compared to seven hours fewer in 2004. The narrowing gap does not surprise Lemire, she says.
“Past surveys and analysis of the national physician survey data have shown that if men and women physicians have no dependents, their hours are almost identical,” she told CMAJ. “We do know that parental responsibilities play a role in the slight decrease in the number of hours that women work in comparison to men.”
Despite reports of the difficulty some residents and newly graduated doctors have in obtaining jobs, the survey indicates that just 1% of doctors were unemployed, while just 5% considered themselves underemployed — some by their own choice.
Broken down by specialty, critical care physicians were most likely to consider themselves underemployed or unemployed, followed by cardiovascular and thoracic surgeons, orthopedic surgeons, general surgeons, nuclear medicine specialists and gastroenterologists. For some of these specialists, underemployment correlated with difficulty getting operating room space.
Just 3% of family doctors considered themselves underemployed, compared to 8% of other specialists. Doctors under 35 reported higher rates of unemployment (1.6%) and underemployment (10%) than the average of all the doctors who completed the survey.
The survey also indicates that — for the first time since it was undertaken — most doctors are now paid by multiple sources, including fee-for-service, capitation based on the number of patients they serve and remuneration for teaching or research.
Most doctors still receive half of their earnings from the fee-for-service model, even if their income comes from a variety of sources. Previously, most doctors were paid that way. Only 8% of physicians are paid primarily by salary.
In another trend, 62% of Canadian doctors are now using some form of electronic health record, up from 39% in 2010.











