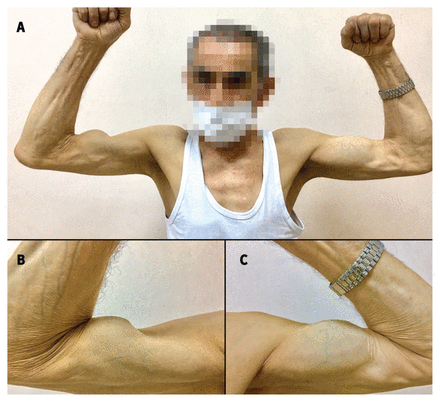
A 70-year-old man presented to our clinic with suddenonset pain and abnormal bulging in his right upper arm. He was a farmer, and reported engaging in strenuous overhead activity, but did not remember any trauma. He had a history of chronic intermittent shoulder pain and a previous diagnosis of tendinitis. On examination, we observed that the belly of the patient’s biceps appeared to bulge more distally on the right than the left (Figure 1). Hand supination was painful and weaker on the right side than the left. We diagnosed rupture of the proximal tendon of the long head of the biceps brachii.
Photographs of a 70-year-old man with biceps tendon rupture. (A) Bilateral comparison with elbow flexion shows hump formation on the right side caused by bulging of the biceps muscle because of proximal rupture, compared with the intact biceps on the contralateral side. Panels (B) and (C) show close-up photographs of the bulging right and normal left biceps muscles, respectively.
The “Popeye sign” observed in our patient is pathognomonic for this condition. We confirmed the diagnosis with magnetic resonance imaging (MRI) of the shoulder, which showed no tendon within the bicipital groove (Appendix 1, available at www.cmaj.ca/lookup/doi/10.1503/cmaj.210948/tab-related-content). We prescribed analgesia with nonsteroidal anti-inflammatory medication, and advised rest and activity modification. We also referred him to physiotherapy for range of motion optimization and strengthening of the rotator cuff and scapular stabilizers.1 At 2-month follow-up, the patient reported occasional arm cramping that did not restrict his activities. He had full range of motion of the shoulder, with a residual bulge formation when he flexed his elbow. Supination was no longer painful and showed no weakness.
Complete proximal biceps tendon rupture occurs more often in older men, usually spontaneously because of tendon degeneration. 1 Its incidence is unknown, but risk factors include smoking, older age, repetitive overhead activities, chronic tendinitis and steroid use or injection.2 It can occur secondary to degeneration and is not always preceded by trauma.
Diagnosis of proximal biceps tendon rupture is clinical and supported by a history of shoulder overuse, chronic tendinitis or rotator cuff disease. After conservative management, if pain and deformity are unresolved on follow-up, clinicians should investigate with ultrasonography or MRI and refer the patient to orthopedics to assess for tenodesis.2,3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/