A 37-year-old man, who had immigrated from Romania 4 years prior, presented to the emergency department after several months of frequent urination and right-sided lumbar pain. Urine microscopy showed leukocytosis and hematuria. His urine bacterial culture was negative and renal function was normal. An abdominal computed tomography (CT) scan showed right kidney abscesses and thickening of the bladder and urethral walls (Figure 1A). He received a diagnosis of complicated upper urinary tract infection (UTI), and was treated with levofloxacin.
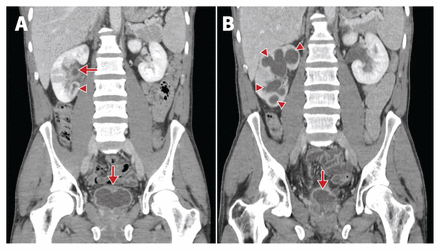
Computed tomography scans from a 37-year-old man with urinary tract tuberculosis. (A) Scan from first presentation, showing an abscess of the lower pole of the right kidney (arrowhead), and thickening of the renal pelvis and bladder walls (arrows). (B) Scan from 3 months after starting treatment for tuberculosis, showing progression of right hydronephrosis (arrowheads) and severe shrinkage of the bladder (i.e., thimble bladder) (arrow).
Six months later, the patient presented again with similar symptoms. Repeat urine culture was negative and he was empirically treated with trimethoprim–sulfamethoxazole. One year after initial presentation, the patient still had urinary tract symptoms. Upon receiving a CT scan for a dental abscess, he was found to have apical pulmonary micronodules with centrolobular distribution.
Given the low prevalence of UTIs in young men, and the patient’s chronic sterile pyuria, failure to respond to antibiotics and pulmonary findings on CT, we suspected genito-urinary tract tuberculosis. He was referred to our infectious disease service. A repeat CT scan showed parenchymal cavitation. Urine testing with auramine staining, showed acid-fast bacilli, and urinary polymerase chain reaction (PCR) and culture were positive for Mycobacterium tuberculosis. We treated the patient with rifampin, isoniazid, pyrazinamide and ethambutol, but he developed partial destruction of renal tissue, ureteral stenosis and severe shrinkage of the bladder (Figure 1B). At 1-year follow-up, he had developed renal impairment, with an estimated glomerural filtration rate of 71 mL per minute.
Genitourinary tuberculosis is the third most common site of infection, accounting for 10% of cases.1 The gold standard for diagnosis is mycobacterial culture from urine, but the organism can take weeks to grow; PCR may provide a quicker diagnosis, with a sensitivity of 89% and a specificity of 95%.2 Prognosis of genitourinary lesions is poor, as they often lead to persistent lower urinary tract symptoms and renal failure.1,3,4 Damage is often irreversible, but reconstructive surgery may mitigate persistent symptoms.1
Clinicians should consider genitourinary tuberculosis in patients who present with sterile pyuria, have risk factors for tuberculosis and fail to respond to standard treatment for UTI.5
Acknowledgement
The authors thank Jessica Peltzer (Department of Anesthesiology, Caen University Hospital, France) for her review of this manuscript’s grammar and syntax.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/