Abstract
Background: Canada has 2 main streams of resettlement: government-assisted refugees and privately sponsored refugees, whereby citizens can privately sponsor refugees and provide resettlement services, including health care navigation. Our objective was to compare receipt of adequate prenatal care among privately sponsored and government-assisted refugees.
Methods: This population-based study used linked health administrative and demographic databases. We included all resettled refugees classified as female who landed in Ontario, Canada, between April 2002 and May 2017, and who had a live birth or stillbirth conceived at least 365 days after their landing date. Our primary outcome — adequacy of prenatal care — was a composite that comprised receipt of a first-trimester prenatal visit, the number of prenatal care visits recommended by the Society of Obstetricians and Gynaecologists of Canada and a prenatal fetal anatomy ultrasound. We accounted for potential confounding with inverse probability of treatment weighting, using a propensity score.
Results: We included 2775 government-assisted and 2374 privately sponsored refugees. Compared with privately sponsored refugees (62.3% v. 69.3%), government-assisted refugees received adequate prenatal care less often, with a weighted relative risk of 0.93 (95% confidence interval 0.88–0.95).
Interpretation: Among refugees resettled to Canada, a government-assisted resettlement model was associated with receiving less adequate prenatal care than a private sponsorship model. Government-assisted refugees may benefit from additional support in navigating health care beyond the first year after arrival.
There are currently about 32.5 million refugees in the world, according to the United Nations High Commissioner for Refugees, 1 and the gap between refugees and available resettlement places is widening.2 In 2020, the United Nations requested that countries increase private sponsorship pathways.3 A dozen countries are exploring private sponsorship,3 and Canada’s private sponsorship pathway has been used as a model for other countries.4
Canada has 2 main streams of resettlement: government-assisted and privately sponsored refugees. Government-assisted refugees are selected by United Nations High Commissioner for Refugees based on higher protection needs and, as a result, have more language, education and health needs.5 In the first year, government-assisted refugees are connected to health care services by government-selected and-funded organizations, but privately sponsored refugees rely on a small group of individuals or established community organizations without formal training in navigating health care.5 Privately sponsored refugees are often sponsored by family members, but those in a private settlement pathway established in 2013, the Blended Visa Office–Referred program, are resettled by nonfamily volunteers.6
Adequate health care is critical to successful integration for refugees, and is particularly important for refugees who are pregnant and at higher risk of adverse outcomes.7 Both refugees in the government-assisted and privately sponsored (including those in the Blended Visa Office–Referred pathway) categories are immediately eligible for provincial health care insurance. Specific health considerations for refugees include premigration exposures and barriers to accessing health services in the country of resettlement.8
Late access and inadequate prenatal care are associated with poor maternal and infant outcomes.9,10 After adjusting for risk factors, Canadian studies have found maternal and neonatal outcomes to be poorer among refugees than among other immigrants and long-term residents.11,12
Our objective was to determine whether refugee sponsorship models in Canada are associated with receipt of adequate prenatal care services, comparing the experience of government-assisted and privately sponsored refugees. Because government-assisted refugees have access to health services facilitated by government services, we hypothesized that, after adjusting for confounding, they would be more likely than privately sponsored refugees to receive adequate prenatal care. To provide context for the findings, we include a comparison with nonrefugee immigrant and long-term resident populations.
Methods
Study design and setting
We conducted a population-based cohort study among resettled refugees in Ontario from 2002 to 2017. We used administrative health care databases for all individuals eligible for government-funded health insurance13 at ICES, a not-for-profit research institute (https://www.ices.on.ca/About-ICES). Ontario is Canada’s most populous province (population around 14 million) and receives about half of Canada’s refugees, of whom more than 98% settle in urban areas.14 Appendix 1, Supplemental Table 1 (available at www.cmaj.ca/lookup/doi/10.1503/cmaj.221207/tab-related-content) outlines selection criteria used to categorize refugees and the support they receive in Canada. We followed Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) and Reporting of Studies Conducted Using Observational Routinely Collected Data (RECORD) reporting guidelines for observational studies using routinely collected data.15,16
Data sources
Data were available from Apr. 1, 2002, to Mar. 31, 2020. All data sets were linked using unique encoded identifiers and analyzed at ICES. Appendix 1, Supplemental Table 2 describes the validated databases we used.17–20 We identified government-assisted and privately sponsored refugees using the immigration category in the Immigration, Refugees and Citizenship Canada (IRCC) database. Deterministic and probabilistic linkage of federal immigration data to the Ontario Registered Persons Database identifies 86.4% of all permanent residents and a higher percentage of refugees.21
Study population
We identified female resettled refugees who had arrived in Ontario between Apr. 1, 2002, and May 31, 2017, and who had conceived a pregnancy more than 365 days after the date they arrived, which resulted in a live or stillbirth. The last date of data collection was Mar. 31, 2020.
We restricted our study to include females with pregnancies after 1 year of resettlement, to capture morbidity and primary care affiliation from health care service use. For people with more than 1 birth, we included only the first birth. We excluded females younger than 13 years or older than 49 years, as well as those with pregnancies conceived by assisted reproductive therapy, as they typically receive extra prenatal care. We excluded recipients of midwifery care because the Ontario health plan billing data do not capture midwifery prenatal visits. We included only individuals residing in an urban area, as they represent more than 98% of resettled refugees in Ontario, and access to rural prenatal care may differ from urban access.14
To provide study context, we created 2 secondary cohorts comprising urban nonrefugee immigrants and, separately, urban long-term residents of Ontario. We included nonrefugee immigrants who arrived in Ontario between Apr. 1, 2002, and May 31, 2017, and long-term residents who conceived their first birth in Ontario between Apr. 1, 2003, and May 31, 2019. See Appendix 1, Supplemental Table 3 for cohort definitions and additional inclusion and exclusion criteria.
Immigration categories
Our exposure was the refugee model (government-assisted or privately sponsored refugee). Because people in the Blended Visa Office–Referred programs receive private sponsorship and comprise a small minority (1%–2%) of resettled refugees to Canada, we assigned them to the privately sponsored refugee category (Appendix 1, Supplemental Table 1).6
Outcomes
Our primary study outcome was receipt of adequate prenatal care according to international and Canadian guidelines.22,23 It was a composite of all 3 of the following: initiation of prenatal care by 13 weeks’ gestation; receipt of a minimum number of prenatal care visits, as recommended by the Society of Obstetricians and Gynaecologists of Canada (SOGC);22 and receipt of a prenatal fetal anatomy ultrasound between 16 and 21 weeks’ gestation. We also analyzed each component separately as a secondary outcome.
Although our composite outcome has not been validated, this outcome reflects local practice guidelines and incorporates a measure of quality through inclusion of ultrasound screening. Like other indices in the literature,24–27 it is predicated on the undisputed benefit of early initiation of prenatal care.22,23 We use the SOGC minimum requirements of prenatal visits (Appendix 1, Supplemental Table 4) to capture adequacy. 22 We used the total number of visits, regardless of the trimester in which care was initiated. The sonographic screening recommended by the SOGC has been shown to reduce adverse pregnancy outcomes.22,28,29
We defined a prenatal care visit as any visit to a family physician, obstetrician or nurse practitioner where a visit was billed to the provincial health plan or identified using electronic medical records at a community health centre. Community health centres deliver primary health care and prioritize immigrant and refugee populations.30 We used billing codes to identify prenatal care visits and receipt of fetal anatomy ultrasound, according to Ontario Ministry of Health billing code definitions31 and previously published work (Appendix 1, Supplemental Table 5).32,33
In addition to the individual components of the primary composite outcome, secondary study outcomes included receipt of adequate care as determined by the Revised-Graduate Prenatal Care Utilization Index (R-GINDEX) and the Adequacy of Perinatal Care Utilization (APNCU) index. The R-GINDEX is based on American College of Obstetricians and Gynecologists’ recommendations and includes the number of prenatal visits, gestational age and initiation of first-trimester care.24,25,27,34 The APNCU index categorizes adequacy based on initiation of care in the first trimester and a ratio of the number of prenatal care visits to the number of expected visits (we used minimum SOGC recommendations to calculate the number of expected visits).22,26
Covariates
We obtained patient demographics (age, parity, neighbourhood income quintile) using hospital records for data accuracy, captured at delivery. Sociodemographic characteristics such as education and ability to speak English or French (self-reported) were captured at time of immigration to Canada using immigration records. The Johns Hopkins ACG System Aggregated Diagnosis Groups case-mix adjustment system (version 10) is commonly used as a comorbidity index.35 We used this index to determine Resource Utilization Bands (health care utilization) and Aggregated Diagnosis Groups (i.e., presence of any major morbidity) in the 1 year before conception, as described elsewhere. 18 We assigned primary care affiliation by billing and rostering data in the year before conception.19 We assigned prenatal care provider based upon visits. Covariates, their definitions and their source databases are available in Appendix 1, Supplemental Table 2.
Statistical analysis
Differences in baseline covariates were assessed using standardized differences (SDs), with a value greater than 0.10 considered potentially important.36
In assessing the study outcomes between the government-assisted and privately sponsored refugee groups, confounding is likely as the distribution of baseline characteristics that affect the outcome differed between the 2 groups of refugees. Accordingly, we used inverse probability of treatment weighting (IPTW) using the propensity score to reduce the effects of confounding.36 The propensity score balances the distribution of measured covariates between the groups. Inverse probability of treatment weighting uses the propensity score to balance baseline patient characteristics by weighting each individual by the inverse of the probability of receiving the actual exposure that was received. We derived propensity scores using a logistic regression model, in which a binary variable denoting resettlement category was regressed on the covariates.
Previous research has shown it is advantageous to include in the propensity score model those variables that are prognostic for study outcomes.37 Accordingly, we included these variables that have been hypothesized or are known to be associated with prenatal care:36 maternal age at conception, parity, time in Canada since immigration, year of delivery, maternal education level at immigration, maternal ability to speak English or French at immigration, secondary migration (arriving from a country other than birth country — a proxy variable for immigration through refugee camps), neighbourhood income quintile, primary care affiliation, Resource Utilization Bands and any major Aggregated Diagnosis Groups. The justification for these variables is outlined in Appendix 1, Supplemental Table 6.
We calculated individual weights using the propensity score: 1/propensity score for government-assisted and 1/(1 – propensity score) for privately sponsored refugees. We estimated relative risks (RRs) in the weighted sample using a modified Poisson regression with a robust variance estimator where confidence intervals (CIs) were calculated using a bootstrap percentile interval with 2000 bootstrap samples.
We did not include region of origin and prenatal care provider in the propensity score, as we do not believe that region of origin (given the diversity of countries and health systems within each region) would be associated with the outcome, and prenatal care provider was measured during the period in which outcomes were ascertained. For comparisons of outcomes among government-assisted versus privately sponsored refugees, and the secondary cohorts, we used χ2 tests with significance set at a 2-sided p value, ≤ 0.05.
We handled missing data (0.2% of the study population) specific to each variable: we merged missing language ability and missing education with the category of “none.” Institutional policy required suppression of cell sizes less than 6 to ensure there was no risk that patients could be re-identified. Accordingly, we merged suppressed neighbourhood income with the lowest quintile, as these neighbourhoods are mostly marginalized.38 Subsequently, we used a complete case analysis approach.
We performed all statistical analyses in SAS version 9.4 (SAS Institute, Cary, NC).
Ethics approval
The use of data in this project was authorized under Section 45 of Ontario’s Personal Health Information Protection Act, which does not require review by a research ethics board.
Results
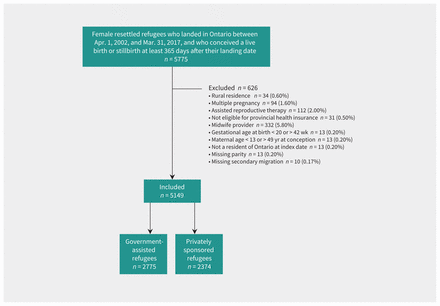
The study included 2775 government-assisted and 2374 privately sponsored refugees, the latter including 102 people in the Blended Visa Office–Referred programs (Figure 1 and Table 1). Before IPTW, privately sponsored refugees were more likely than government-assisted refugees to have a higher education and ability to speak English or French, reside in a higher income area, and be less likely to have a major comorbidity. After IPTW, as expected, baseline differences between the groups were small (Table 1), which indicates that the propensity score model was adequately specified.
Flowchart of participant inclusions and exclusions.
Characteristics of government-assisted and privately sponsored refugees
Primary outcome
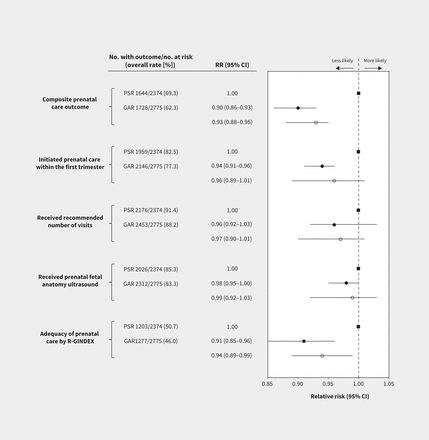
The rate of receipt of adequate prenatal care was 62.3% among government-assisted refugees and 69.3% among privately sponsored refugees, corresponding to an unweighted RR of 0.90 (95% CI 0.86–0.93) and a weighted RR of 0.93 (95% CI 0.88–0.95) (Figure 2).
Receipt of adequate prenatal care and related outcomes, comparing government-assisted refugees (GAR; circles) with privately sponsored refugees, the reference category (PSR; squares). The composite prenatal care outcome comprised the receipt of a first-trimester visit, the recommended number of prenatal visits and a prenatal fetal anatomy ultrasound. The black circles reflect the unweighted analysis, and the white circles the inverse probability treatment–weighted analysis, the latter based on a propensity score that included maternal age, parity, year of delivery, education, language ability, neighbourhood income quintile, primary care affiliation, resource utilization band and the presence of a major maternal comorbidity. Note: CI = confidence interval, R-GINDEX = Revised-Graduated Prenatal Care Utilization Index, RR = relative risk.
Secondary outcomes
The individual components of the composite outcome were lower among government-assisted than privately sponsored refugees, but neither receipt of a first-trimester visit nor the number of prenatal care visits was significantly different after IPTW (Figure 2). Findings were similar for receipt of prenatal ultrasound.
The mean number of prenatal care visits for government-assisted refugees was 12.0 (SD 4.3) and 11.4 (SD 4.7) for privately sponsored refugees (p < 0.01) and the mean number of ultrasounds was 3.0 (SD 2.0) for government-assisted refugees and 2.8 (SD 1.9) for privately sponsored refugees (p = 0.05). Government-assisted refugees were less likely to receive adequate care than privately sponsored refugees, as determined by the R-GINDEX (46.0% v. 50.7%; weighted RR 0.94, 95% CI 0.89–0.99) (Figure 2) and the APNCU index (Appendix 1, Supplemental Table 8).
Adequate care in nonrefugee immigrants and long-term residents
Characteristics in the secondary cohorts (557 950 long-term residents and 105 099 nonrefugee immigrants) are shown in Appendix 1, Supplemental Table 7. Compared with long-term residents, government-assisted refugees were less likely to have the composite prenatal care outcome (69.0% v. 62.3%; RR 0.90, 95% CI 0.88–0.93) and nonrefugee immigrants were more likely (69.0% v. 71.6%; RR 1.04, 95% CI 1.03–1.04), with no difference for privately sponsored refugees (69.0 v. 69.3%; RR 1.01, 95% CI 0.99–1.04) (Table 2).
Prevalence of adequate prenatal care, and related outcomes, among government-assisted refugees, privately sponsored refugees and the secondary cohorts of nonrefugee immigrants and long-term residents in Ontario*
Using the R-GINDEX, we found that all refugee and nonrefugee immigrant groups were more likely than long-term residents to receive adequate prenatal care (Table 2); we saw similar results for the APNCU index (Appendix 1, Supplemental Table 9).
Interpretation
This population-based study in Ontario, Canada, found that government-assisted refugees were less likely to receive adequate prenatal care services than privately sponsored refugees, after we performed propensity score weighting to reduce confounding potentially introduced by the immigration selection process.
Our findings suggest that private sponsorship plays a role in facilitating prenatal care use, and that government-assisted refugees may benefit from additional resettlement support related to health care navigation. A lower proportion of government-assisted than privately sponsored refugees had a first-trimester visit and received a fetal anatomy ultrasound; however, after reducing confounding, government-assisted refugees had a relative risk similar to that of privately sponsored refugees for both outcomes.
This attenuation in the weighted results suggests that government-assisted refugees may have barriers to accessing prenatal care related to factors included in the propensity score, such as education and language ability. This finding could help target services to improve health care access, especially after the onset of the COVID-19 pandemic.
Although we found a statistically significant difference with the composite score, none of the individual components were different between the 2 groups after IPTW. This may be because our sample size was too small to detect a difference and it may also indicate that people who receive 1 component of care may not receive another.
We found effect sizes with the composite outcome that were close to that of the R-GINDEX. The R-GINDEX is driven mostly by the number of prenatal visits, and the populations most likely to have had an adequate number of visits also had adequate care as measured by the R-GINDEX (Table 2) and APNCU index (Appendix 1, Supplemental Table 9).
Privately sponsored refugees and nonrefugee immigrants were more likely to have an adequate number of visits than long-term residents. The indices do not capture the content of the visits; however, increased visits related to perceived or higher medical need or need for counselling may be reasons for more visits in the privately sponsored refugees and nonrefugee immigrant populations. There is limited evidence on the relationship of the R-GINDEX and APNCU index to outcomes.27
Evidence suggests that private sponsors remain committed after 1 year of resettlement and can act as cultural brokers.39 A single-centre study showed privately sponsored refugees were more likely to complete cervical screening than government-assisted refugees despite being offered this screening at the same rate.40 This suggests that our findings on ultrasound use may not reflect access to care alone. Our data do not allow us to identify factors such as differing attitudes toward fetal screening; this may affect the acceptance of fetal anatomy ultrasounds.9,10,41 The same group studied refugees who were pregnant upon arrival in Canada and showed that government-assisted refugees received higher rates of first-trimester visits than privately sponsored refugees.42 These findings likely reflect higher screening rates in newly arrived government-assisted refugees by refugee specialists who are aware of their higher medical needs.
Limitations
We excluded those with pregnancy loss before 20 weeks’ gestation, estimated at 8%–10% in a Canadian population.43 We excluded them because of the shorter gestation period and the complexity of factors associated with pregnancy loss.
Midwifery visits are not included in the billing data available to us, despite midwives being an important source of prenatal care in Ontario.44 Patients with midwifery visits not documented in the hospital delivery record may have been included, which may have underestimated the extent of prenatal care; this is another reason that some patients may have received 1 component of recommended prenatal care but not another. A minor percentage (n = 88 [0.01%]) of patients had no physician billing claims and a small percentage (n = 2320 [0.3%]) had no prenatal visits despite having a hospital delivery, which may reflect uncaptured prenatal care.
There have been no validation studies of the refugee category variable in the immigration data. Our primary outcome and identification of prenatal visits by billing codes is not validated and may misclassify visits as prenatal care, or under-capture visits that included prenatal care content with alternative billing codes; this could affect our estimation of timing of initiation. We were unable to measure the content or quality of visits.
Conclusion
Among resettled refugees in Canada, those in the government-assisted pathway were less likely to receive adequate prenatal care than privately sponsored refugees. Government-assisted refugees may benefit from longer-term resettlement support related to health care navigation, even in a health care system that publicly funds all physician care and hospital admissions.
Footnotes
Competing interests: Andrea Evans was funded by the Frederick Banting and Charles Best Canadian Institutes of Health Research Scholarship and the Ontario Women’s Research Health Scholars Award. Astrid Guttmann reports holding a Tier 1 Canada Research Chair and was the nominated principal applicant of grant no. PJT-155917, awarded by the Canadian Institutes of Health Research. Peter Austin is supported by a Mid-Career Investigator Award from the Heart and Stroke Foundation (paid to institution). No other competing interests were declared.
This article has been peer reviewed.
Contributors: Andrea Evans, Astrid Guttmann, Joel Ray and Peter Austin contributed to the conception and design of the work. Andrea Evans, Astrid Guttmann and Hong Lu contributed to the acquisition, analysis and interpretation of data. Andrea Evans drafted the manuscript. All of the authors revised the manuscript critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health. This study also received funding from the Canadian Institutes of Health Research grant no. PJT-155917. All decisions regarding study design, publication, and data analysis were made independent of the funding agencies. The study funder had no role in study design, data collection, data analysis, data interpretation or writing.
Disclaimer: Parts of this material are based on data and information compiled and provided by the Ontario Ministry of Health, Canadian Institute for Health Information and Immigration, Refugees and Citizenship Canada (IRCC) current to May 31, 2017. Geographical data are adapted from Statistics Canada, Postal Code Conversion File +2011 (Version 6D) and 2016 (Version 7B). The analyses, conclusions, and opinions and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement is intended or should be inferred.
Data sharing: The data set from this study is held securely in coded form at ICES. While data-sharing agreements prohibit ICES from making the data set publicly available, access may be granted to those who meet prespecified criteria for confidential access, available at http://www.ices.on.ca/DAS. The full data set creation plan and underlying analytic code are available from the authors upon request, understanding that the computer programs may rely upon coding templates or macros that are unique to ICES and are therefore either inaccessible or may require modification.
- Accepted January 31, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/