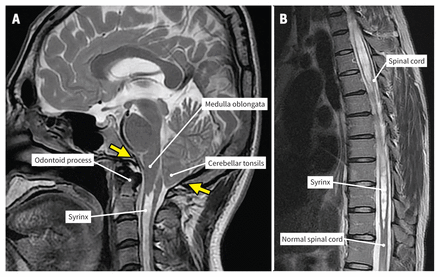
A 33-year-old man presented to our hospital with a 2-week history of dizziness and gait disturbance and a 7-day history of hiccups that persisted throughout the day accompanied by nausea and decreased appetite. The patient had no remarkable medical history, reported no medication or substance use and had no history of hiccups. On physical examination, muscle strength and tendon reflexes in the extremities were normal; however, we observed both dysmetria of the right hand and ataxic gait, indicative of a cerebellar disorder. Magnetic resonance imaging of the head showed displacement of the cerebellar tonsils below the foramen magnum level, with a syrinx extending from the C1 to T11 level (Figure 1). We diagnosed Chiari type I malformation and syringomyelia. The patient then underwent foramen magnum decompression including suboccipital craniectomy and C1 laminectomy. After surgery, he had gradual improvement in symptoms; after 2 months, his symptoms, including the hiccups, disappeared and the syrinx cavity size was reduced on follow-up imaging.
(A) Midsagittal T2-weighted magnetic resonance imaging (MRI) scan of the brain and brainstem of a 33-year-old man showing the cerebellar tonsils displaced into the upper cervical canal, 8 mm below the foramen magnum (basion-opisthion line, arrows), with slight caudal descent of the brainstem and effacement of cerebrospinal fluid space. Although retroflexion of the odontoid process, shortened clivus and small basilar invagination (the odontoid process lies 6.2 mm across the Chamberlain line) were observed, there was no compression of the brainstem. A cervical syrinx formation was also seen. (B) Midsagittal T2-weighted MRI scan of the thoracic spine showing a syrinx extending to the level of T11.
Chiari type I malformation is a hindbrain abnormality in which the cerebellar tonsils descend through the foramen magnum, with a radiological prevalence of 1%–3.6%.1 Frequently asymptomatic, it can present in children and adults with occipital headache, weakness or cerebellar signs. Hiccups are an uncommon presentation.2 Hiccups arise from stimulation or damage to the hiccups reflex arc, comprising the hypothalamus, brainstem, cervicothoracic spinal cord, vagal and phrenic nerves and respiratory muscles.2,3 Both Chiari malformation and concomitant syrinx (a fluid-filled cavity involving the brainstem [syringobulbia] or spinal cord [syringomyelia]), can affect the hiccups reflex arc, leading to hiccups.2,3 Syringomyelia is present in about 25% of patients with Chiari type I malformation.1 Although typically self-limiting, hiccups lasting longer than 48 hours may require investigation for an underlying cause.2,3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/